Testing the Waters: How one behavioral health group is benefitting from AI

As we discussed in our recent white paper, the use of Artificial Intelligence in Behavioral Healthcare is still in its infancy—but we expect growth to happen soon, and quickly. Given the current state, though, we’ve gotten dozens of questions from our clients about what adopting and implementing AI looks like.
We spoke to our colleagues at All Points North (APN), a multi-site, 77-bed Behavioral Health system based in Colorado, who decided to move ahead with an AI solution. APN was already using Kipu’s EMR, so they chose to go with Eleos, which is integrated with the Kipu EMR. Eleos focuses on supporting documentation and note taking in therapeutic sessions through their AI solution, which was a key area APN was hoping to improve.
“Many of our treatment centers were struggling with documentation,” Andrea Boorse, senior manager of operations at APN, shared. APN clients have two individual therapy sessions each week, rather than one—which means double the documentation. When they became aware of AI solutions that could listen in on sessions and help with that documentation, they decided to test the waters—with Eleos’s Scribe solution, which automatically transforms raw conversations into progress note suggestions.
Getting buy in, seeing results
Since APN was essentially the guinea pig for the solution, they expected a few bumps along the way. Fortunately, they found that those bumps came along a lot less frequently than they anticipated. “There were a few bugs and issues at first,” Andrea said—but the biggest challenges were getting buy-in from clients and providers.
“We had to figure out the best way to explain this to clients to get them comfortable. When they hear that a bot will be listening in on their session, it can undermine trust before the therapist really has a chance to establish it. But we’ve found that once clients understand that this will allow the therapist to be more present during sessions, helping to improve the quality of therapy over time, they tended to be all in.”
In addition, while APN presented the tool as part of their therapy process, if any client expresses that they do not want it used during sessions then they opted out of using the tool.
Providers were a different story. A lot of the clinicians weren’t buying in at first, so APN incentivized adoption. Andrea instituted an OKR (objective and key result). “I wanted at least 90% of individual sessions to be done with the tool so we could really see if it was useful and working,” Andrea said. “And the cool thing is, the more we use it, the more it learns, and the better it gets.”
For example, they found that there’s a major leap in the quality of the notes and summaries after roughly 20 sessions with a therapist. “The tool starts to understand and recognize therapists’ style and language, making the notes get more specific and tailored to each client,” Andrea shared. This has been a big help for APN–it now takes an average of 11 minutes to complete a note, compared to the industry standard of 15 minutes.
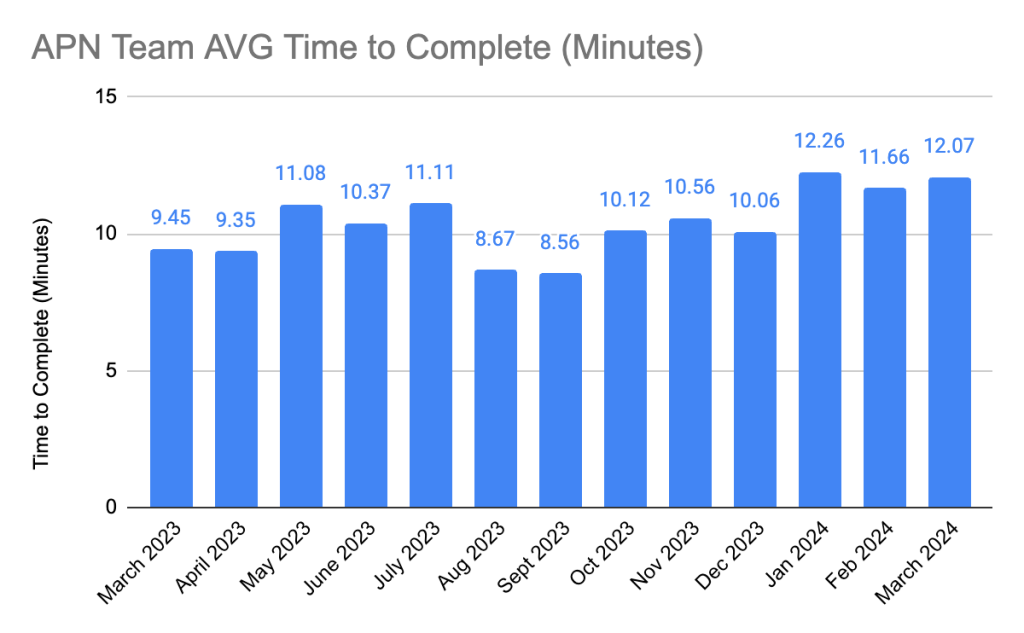
Above: the average time documentation took per visit at APN since rolling out Scribe. All in all, the team has saved more than 110 hours since implementing Scribe.
That’s not to say there still aren’t issues and barriers. For instance, APN has decided to hold off on using the tool in any group therapy sessions. There are a few reasons why:
- Opting out: If even one patient doesn’t want to have the tool in use, they cannot use it at all.
- Technology challenges: While the tool works well in individual sessions, APN found that it had some trouble picking up individual voices, or getting names right in the notes and transcriptions.
- Perception: Clients are generally less comfortable with using the tool in a group
Improving alignment, quality, and getting a competitive advantage
Making the choice to focus on the AI’s efficacy in one-on-one therapy sessions is benefiting APN—especially in therapeutic alignment, the quality of notes, and in helping get a slight edge in recruiting younger therapists.
- Therapeutic alignment: When therapists use the tool, it means they aren’t looking down at a notepad, which can lead to a feeling of disconnection for the client. “The clients feel more heard, because they feel the therapist is focusing more on them. The therapist is making more eye contact, and clients can see that their therapists are more open and present,” Andrea shared.
- Quality of notes: When therapists use the tool consistently, something interesting starts to happen: the tool recognizes themes and patterns, which can reveal gaps or insights that weren’t noticed previously. It’s also helping uncover more information, which leads to an additional benefit: “The amount of information we’re getting is just so much more than you know writing a few sentences. The quality of information has improved, which helps us with documentation with payors,” Andrea noted.
- Competitive recruitment: APN has also noticed that younger applicants to therapy positions are attracted to the fact that APN uses AI to help documentation, helping APN find and recruit top talent.
What to consider for adopting AI
APN has learned a lot since they first implemented the tool in 2022. Here’s a few lessons learned that Andrea shared:
- Ensure it integrates with your EMR: A tool that’s fully integrated into the EMR makes adoption easier. “It just makes the process easier to have it right there,” says Andrea.
- Ensure the tool has excellent customer support: And for tools like these, good customer support doesn’t just mean having a great support manager. “You really do need a team supporting you—even if it’s just a couple of people—to help you troubleshoot on the fly. The most effective deterrent for people using a product is its frequent malfunctions, leading to increased time expenditure and rising frustration levels.”
- Create Internal champions: Find one staff person at least who will be your initial power user. Make sure they’re interested and excited and let them find out as much as they can about how a tool works. Then, use their enthusiasm and understanding of issues or challenges to bring the rest of your staff onboard.
As we shared in our white paper, deciding when or if to adopt an AI solution is a complex decision. Make sure you inform yourself on the pros and cons of any tool. If you need more information or support, visit us at kipuhealth.com.
Rely on Kipu to keep you ahead of change.
Subscribe to Kipu for behavioral health news, updates, community celebration, and product announcements.



