RCM – Stronger Revenue for Stronger Care

Get Paid Faster and Reinvest In Your Practice
From pre-admission to post-discharge, Kipu RCM embeds the necessary workflows and payer requirements along each step of the patient journey to ensure claims are submitted and paid as accurately and quickly as possible.
By integrating with Kipu EMR, teams save time and reduce human-error by pushing patient demographics and charges seamlessly to the billing software with one click.
Kipu RCM cleanly submits nearly 1.5 million claims annually.
- Up to 99% Perfect Pass, and Clean After Waystar Rate
- Clearinghouse Rejection rate as low as 0.44%
- Payer Rejection Rate as low as 0.21%
See How Much Money You’re Missing
This calculator helps you assess what’s slipping through—and what you could gain with a better revenue cycle management strategy.

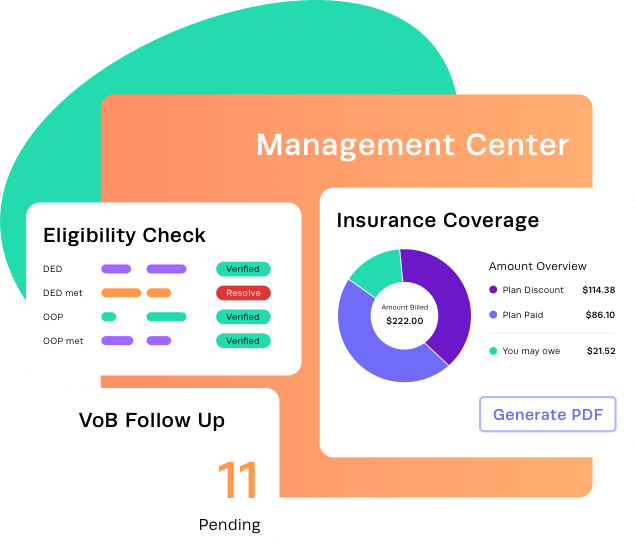
Simplify the process of verifying patient eligibility and benefits for faster reimbursement.
With our comprehensive Management Center, you can conveniently handle all aspects of eligibility and benefit verification in a single centralized location.
Say goodbye to time-consuming tasks and enjoy streamlined operations that pave the way for a healthy revenue cycle.
Detailed coverage information
Quickly access detailed coverage info in a user-friendly PDF via electronic eligibility checks, no hassle, no guesswork.
Verification
Track and prioritize benefit exceptions with the Management Center to stay on top of follow-ups and coverage issues.
Eligibility Check
Run real-time or scheduled batch eligibility checks for all active patients with ease.
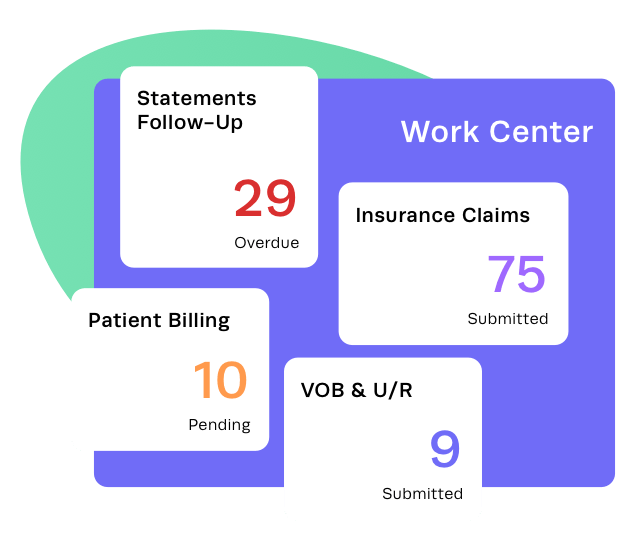
Utilization Review reduces the time between patient treatment and reimbursement
Our user-friendly system ensures that your facility stays updated with the latest authorizations, streamlining the U/R process for optimal efficiency.
Dashboard alerts
Prevent revenue gaps before they occur with color-coded dashboard alerts for new, incomplete, and expired or soon-to-be-expired utilization reviews.
Authorization alerts
Keep on top of authorizations through proactive alerts, ensuring timely updates.
Utilization plans
Create Utilization Plans directly from the patient’s treatment episode or within the U/R Work Center for easy reference.
Task management
Assign and track tasks to team members for efficient follow-up on important items.
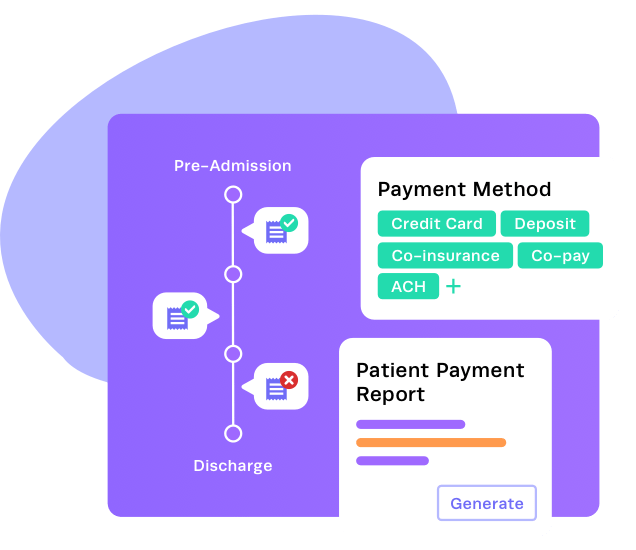
Eligibility and Verification of Benefits
Collection alerts at the right moments during the patient journey ensures timely payment processing while delivering a smooth patient financial experience.
Payment collection
Collect proper payment at any point in the patient journey—including pre-admission.
Payment reports
Reconcile bank deposits with the Patient Payment Report.
Payment options
Enhance convenience for both patients and your staff by accepting various types of payments.
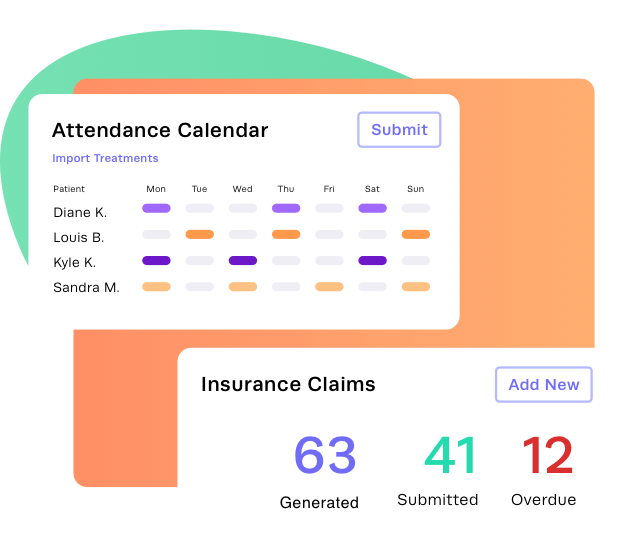
Automate claim creation with the Attendance Calendar
Experience streamlined treatment management and improved efficiency with our user-friendly Attendance Calendar.
Services rendered automation
Automatically populate the Attendance Calendar with services rendered from the Kipu EMR or bulk importing treatments.
Claim automation
Generate claims automatically and with precision using the information from the Attendance Calendar.
Claims management
Correct and void claims quickly to enhance accuracy and ensure timely payment.

Accurate and Up-to-Date Billing
Our comprehensive software and trusted clearinghouse partners eliminates the complexities of enrollments, automate payment posting, and streamline claims management.
Claims creation
Easily create claims and submit them to payers with information coming directly from the Kipu EMR and Attendance Calendar.
Payment insight
Review and analyze payments in bulk or dive into individual payments and provider-level adjustments for detailed insights.
Payer enrollments
Automate ERA posting, process insurance card payments, or record manually as needed.
Custom rules
Customize claim rules to ensure compliance with the requirements of even the most meticulous payers.
Payer management
Streamline the management of payer rates and fee schedules through simple uploads.
Provide a seamless financial experience without the hassle
Our all-inclusive platform empowers you to efficiently manage every aspect of patient billing and collections from a single location.
Effortless statements
Generate easy-to-understand patient statements for your organization or individual patients, with the ability to email them directly from the application.
Task management
Manage and prioritize follow-up tasks through color-coded alerts on the dashboard.
Payment options
Convenient patient payment acceptance options that ensure a smooth and efficient payment process.
Automated follow-ups
Automated follow-up processes that help increase payment compliance and accelerate revenue recovery.

Optimize self-pay revenue
Our software offers convenient self-pay options that are readily available. With our user-friendly workflows, you can easily generate patient statements, collect payments at the right time, and effectively track and compare self-pay revenue to insurance revenue.
Statement transparency
Promote transparency with patients through customized comprehensive statements.
Patient profiles
Build comprehensive self-pay patient profiles, allowing for accurate tracking and management of self-pay accounts.
Flexible payment options
Simplify payment collection with flexible options such as a securely stored credit card and ACH.
Kipu RCM’s reporting dashboards
Quickly identify trends, potential issues, and critical metrics that impact patients, staff, and revenue. Our library of specialized reports is tailored to meet the needs of behavioral health businesses, and you can easily export data to Excel for further analysis.
Instant insights
Accelerate your data analysis with pre-built reports specifically designed for addiction treatment and behavioral facilities.
Comprehensive reports
Gain a comprehensive overview by accessing combined reports that include both insurance and self-pay data.
Efficient reporting
Customize reports to focus on the specific information you need and create report templates for consistent and efficient reporting.
Comparison snapshots
Compare data across different time periods—such as months, quarters, or years—with accurate and detailed period-close snapshot reports.
Kipu’s RCM solution provides expertise, insights, and analytics to move you forward.
Let’s chat more about how you can keep ahead with Kipu.